MASLD in the oldest-old: lack of association with cognition or functional autonomy and poor predictive utility of the hepatic steatosis index
Abstract
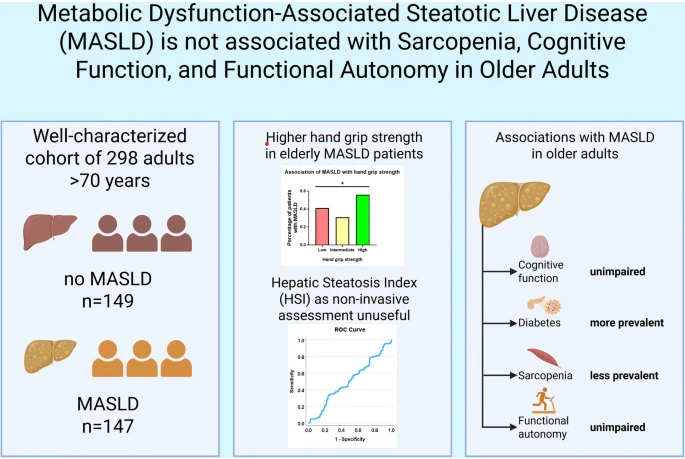
Metabolic dysfunction-associated steatotic liver disease (MASLD) is a prevalent condition increasingly recognized in aging populations. However, its clinical relevance in older adults-particularly in relation to sarcopenia, cognitive function, and rehabilitation outcomes-remains poorly defined. This retrospective observational study included in-patients admitted for geriatric rehabilitation in 2022 with available abdominal ultrasound. MASLD was defined according to AASLD/EASL criteria. Demographics, comorbidities, medications, and the hepatic steatosis index were recorded. Cognitive function (MMSE, clock-drawing, GDS), hand grip strength, mobility (Tinetti, Timed Up and Go), and functional status (Barthel Index, discharge autonomy) were assessed. Analyses included regression and AUROC, with significance at p below 0.05. MASLD was present in 49.6% of the study population. No significant association was observed between MASLD and cognitive impairment. Patients with higher hand grip strengths showed higher proportions of MASLD (p = 0.01). In this cohort, hepatic steatosis index has poor capacity to detect hepatic steatosis (AUC = 0.503, 95%-CI: 0.437-0.570). Furthermore, MASLD did not predict poorer functional outcomes following the rehabilitation stay. In adjusted models, Barthel Index -but neither MASLD nor hand grip strength- was independently associated with reduced functional autonomy at discharge (p = 0.006). In elderly patients, MASLD was associated with diabetes mellitus and higher hand grip strength, while sarcopenia was linked to a lower prevalence of steatosis. MASLD showed no association with cognitive performance, functional outcomes, or prediction by the hepatic steatosis index. These findings highlight age-specific characteristics of MASLD requiring tailored clinical approaches.
